Welcome back to Part 2 of this blog series on hip pain! In Part 1, we explored lateral hip pain,
often tied to muscular issues. This time, we’ll focus on groin pain—felt in the crease between
the stomach and the upper thigh. Groin pain is commonly associated with hip joint problems
such as arthritis, hip impingement, or hip instability/dysplasia. Occasionally, it can radiate from
the upper lumbar spine or anterior hip muscles (like your adductors or hip flexors). While these
muscle-related causes are somewhat common, they’re less frequent than joint-related issues
and will be addressed in a future post.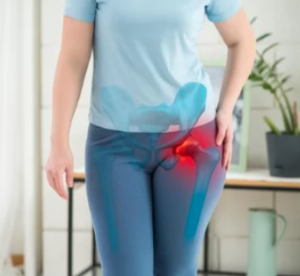
Hip Impingement
Hip impingement occurs when soft tissue gets compressed between the head of the femur and
the hip socket. This happens either due to excessive bone growth on the femoral head (a CAM
lesion) or when the hip socket/labrum covers too much of the femoral head, causing contact
with the tissue during hip flexion. Hip impingement is often seen in younger individuals,
particularly athletes.
Symptoms include anterior hip pain triggered by activities requiring deep hip flexion, such as
squatting, sitting on a low surface, or pulling the knees to the chest during stretching.
How is hip impingement managed?
We focus on improving joint mobility with manual therapies like hip joint manipulations and
self-mobilization techniques (check out our Instagram for ideas!). Next, we emphasize
strengthening exercises for the glutes and, depending on individual deficits, the hip flexors.
Abdominal strengthening is also crucial—it prevents excessive anterior pelvic tilt, which can
exacerbate impingement.
Hip Arthritis
Osteoarthritis of the hip is another common diagnosis, especially in individuals aged 55 and
older. Those with arthritis often experience pain and stiffness that's worse in the morning but
improves after 30–60 minutes of activity. However, pain tends to return with prolonged
activities like walking, gardening, or standing.
What’s the best approach for arthritis?
Manual joint mobilizations to reduce stiffness, combined with a global exercise program
focusing on functional movements—such as squats, step-ups, and lunges—can help maintain
mobility and delay the need for hip replacement as long as possible.
Hip Instability/Dysplasia
Unlike impingement, hip dysplasia occurs when the hip socket doesn’t adequately cover the
femoral head, leading to poor joint stabilization. Individuals often present with groin and lateral
hip pain and a sensation of tightness—not actual tightness, though.
Why the sensation of tightness?
Since the hip joint lacks proper stability, the surrounding muscles, especially anterior hip
muscles and hip flexors, work overtime to compensate. This overwork leads to fatigue and the
sensation of tightness.
What’s the solution for hip instability/dysplasia?

Strengthening the hip flexors, glutes, and adductors is key. Building resilient muscles provides
stability to the hip joint without overloading the musculature. To enhance recovery and
tolerance for daily activities, exercises are paired with manual therapies like soft tissue
mobilization (rather than joint mobilization) and often dry needling. These treatments reduce
pain and alleviate the sensation of tightness, making exercises and day-to-day activities more
manageable.
 Back or side of the hip pain is often linked to muscular or tendon issues, such as gluteal
Back or side of the hip pain is often linked to muscular or tendon issues, such as gluteal

 like to watch you perform the painful movement. This could be squatting, benching, overhead lifting/pressing, etc. Then we’ll perform some therapeutic modalities such as dry needling or perform some soft tissue mobilization, and then come up with some modifications to reduce pain during the exercise, determine an appropriate level of pain to work through (if needed), create a home exercise program, and a schedule to get you back to your prior level of exercise. We also like to work with any other health care worker or fitness professional you’re working with. This will allow us to communicate an individualized plan to keep you in the gym while you go through your rehab journey!
like to watch you perform the painful movement. This could be squatting, benching, overhead lifting/pressing, etc. Then we’ll perform some therapeutic modalities such as dry needling or perform some soft tissue mobilization, and then come up with some modifications to reduce pain during the exercise, determine an appropriate level of pain to work through (if needed), create a home exercise program, and a schedule to get you back to your prior level of exercise. We also like to work with any other health care worker or fitness professional you’re working with. This will allow us to communicate an individualized plan to keep you in the gym while you go through your rehab journey! of repetitive high-speed twisting of the spine after all. While rotation of the spine has gotten a bad rap over the years, when done too much or with other underlying issues, back pain can rear its ugly head. To make things more difficult, the issue might be from something other than the back like the hips, shoulders, or the wrists. That’s why it’s so important to work with someone trained in evaluating golfers. This post is the introduction of series of posts highlighting some common causes of low back pain including certain swing characteristics such as reverse spine angle during the backswing, hip hiking during the downswing, flying elbows, and more.
of repetitive high-speed twisting of the spine after all. While rotation of the spine has gotten a bad rap over the years, when done too much or with other underlying issues, back pain can rear its ugly head. To make things more difficult, the issue might be from something other than the back like the hips, shoulders, or the wrists. That’s why it’s so important to work with someone trained in evaluating golfers. This post is the introduction of series of posts highlighting some common causes of low back pain including certain swing characteristics such as reverse spine angle during the backswing, hip hiking during the downswing, flying elbows, and more. we can determine what factors of the screen are leading to certain swing characteristics which may lead to low back pain. This will help decide if you need to see a medical professional to correct any physical faults or see a golf pro for some lessons. If PT is appropriate for you, we’ll begin with treatment on day one. Day one will include personalized exercises to address any deficits found in the screen along with some manual intervention such as spinal manipulations, soft tissue mobilization, or dry needling. These manual interventions will help reduce pain quickly to get you back to golf ASAP while we also work on strengthening and mobility to prevent the issue from returning in the future. We’ll also get you set up with a golf professional if needed.
we can determine what factors of the screen are leading to certain swing characteristics which may lead to low back pain. This will help decide if you need to see a medical professional to correct any physical faults or see a golf pro for some lessons. If PT is appropriate for you, we’ll begin with treatment on day one. Day one will include personalized exercises to address any deficits found in the screen along with some manual intervention such as spinal manipulations, soft tissue mobilization, or dry needling. These manual interventions will help reduce pain quickly to get you back to golf ASAP while we also work on strengthening and mobility to prevent the issue from returning in the future. We’ll also get you set up with a golf professional if needed.